Question
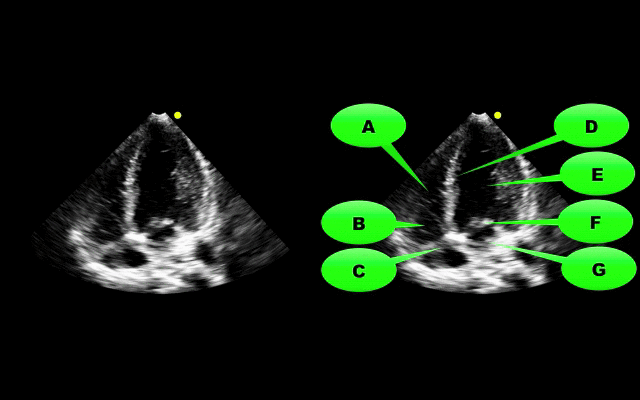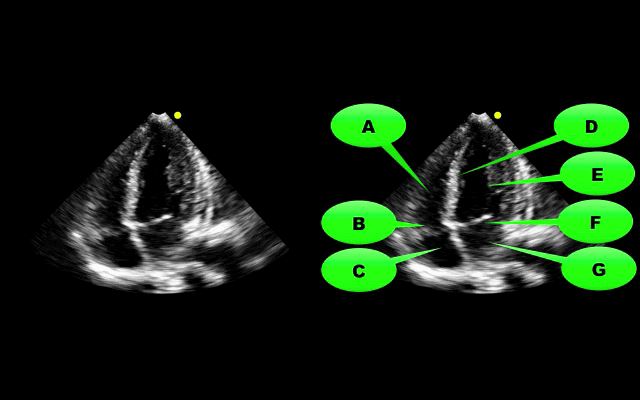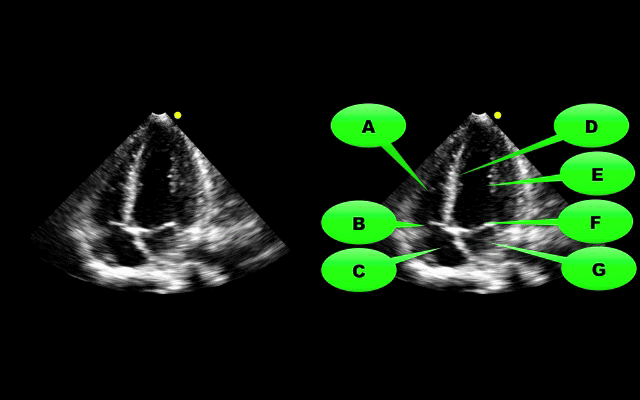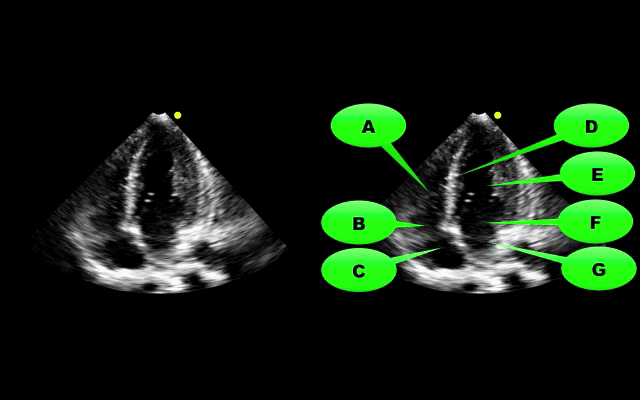
What view of the heart is this and can you name everything from A-G?
Bottom Line: In a stable pediatric abdominal trauma victim, combined FAST and LFT results are an effective screening tool to evaluate for intra-abdominal injury.
The management of alcohol withdrawal syndrome (AWS) includes supportive care focusing on the ABC’s and administration of benzodiazepines (BDZ).
While BDZ are effective in the treatment of AWS, some patients may require very high doses of BDZ to control symptoms (tachycardia, hypertension, diaphoresis, etc.); unfortunately, high-doses of BDZ may lead to suppression of the respiratory drive and endotracheal intubation.
Dexmedetomidine (DEX) is a sedative agent that is an intravenous alpha2-agonist (it's like clonidine); it reduces sympathetic outflow from the central nervous system and it may help treat withdrawal syndromes. The major benefit of DEX is that it does not suppress the respiratory drive, thus intubation is not required.
Smaller trials and case series have shown that patients with AWS who were treated with BDZ in addition to DEX had better symptom control, lower overall BDZ doses, and less respiratory depression/intubation.
Bottom-line: While more trials are needed, consider adding DEX for patients with AWS who require high-doses of BDZ.
What view of the heart is this and can you name everything from A-G?

Want more emergency cardiology pearls? Follow me @alifarzadmd
Unexplained respiratory symptoms during exercise are often incorrectly considered secondary to exercise induced asthma/bronchospasm.
An important diagnosis on the differential should be exercise-induced laryngeal obstruction (EILO).
Of 91 athletes referred for asthma workup, 35% had EILO.
The presence of inspiratory symptoms did not differentiate athletes with and without EILO.
61% of athletes with EILO used regular asthma medication at referral.
Reversal of the new anticoagulants rivaroxaban (Xarelto) and dabigatran (Pradaxa) has been challenging particularly in the ED setting with no definitive reversal agent. Intracerebral hemorrhage or critical GI bleed management becomes challenging and worsens mortality.
There is growing literature that states activated prothrombin complex concentrate or non-activated PCC may reverse these new anticoagulants. A volunteer study (1) showed its efficacy and concensus workgroups are now recommending aPCC as first line therapy(2). The search goes on for a reliable reversal agent for these new anticoagulants which were suppose to solve more problems instead of create new ones.
General Information:
Nisseria meningitidis is the common culprit in epidemic meningitis. Serogroup B is currently causing an outbreak on the Princeton campus. So what are the serogroups and why are they important?
Six main serogroups cause disease: A, B, C, Y, X, W-135.
Two quadrivalent vaccines are currently licensed in the US that cover Serogroups A, C, Y, and W-135.
Relevance to the EM Physician: The currently available vaccines in the US cover the majority of serogroups of meningococcus, however, Serogroup B (currently causing an outbreak at Princeton) is not covered, nor is Serogroup X (for travelers to Sub-Saharan Africa).
Bottom Line: Serogroups B and X are not covered by the currently available vaccines in the US and at risk populations (and physicians treating those patients) should be made aware of the gap in coverage. Investigations for a vaccine for Serogroup B (licensed in Europe and Australia, but not in the US) are currently underway.
University of Maryland Section of Global Emergency Health
Author: Andi Tenner, MD, MPH, FACEP
Ottawa Rules for Subarachnoid Hemmorhage (SAH)
Background
Design
Results
132 (6.2%) had SAH
Decision rule including any:
Had 98.5% sensitivity (95% CI, 94.6%-99.6%) and 27.5% specificity (95% CI, 25.6%-29.5%)
Adding “thunder-clap” headache and “limited neck flexion on examination” (inability to touch chin to chest or raise the head 8cm off the bed if supine) resulted in 100% (95% CI, 97.2%-100%) sensitivity.
The rule was then evaluated using a bootstrap analysis on old cohort data to validate the rule.
Conclusion/Limitations
For alert patients older than 15 y with new severe nontraumatic headache reaching maximum intensity within 1 h
Not for patients with new neurologic deficits, previous aneurysms, SAH, brain tumors, or history of recurrent headaches (≥3 episodes over the course of ≥6 mo)
Investigate if ≥1 high-risk variables present:
Age ≥40 y
Neck pain or stiffness
Witnessed loss of consciousness
Onset during exertion
Thunderclap headache (instantly peaking pain)
Limited neck flexion on examination
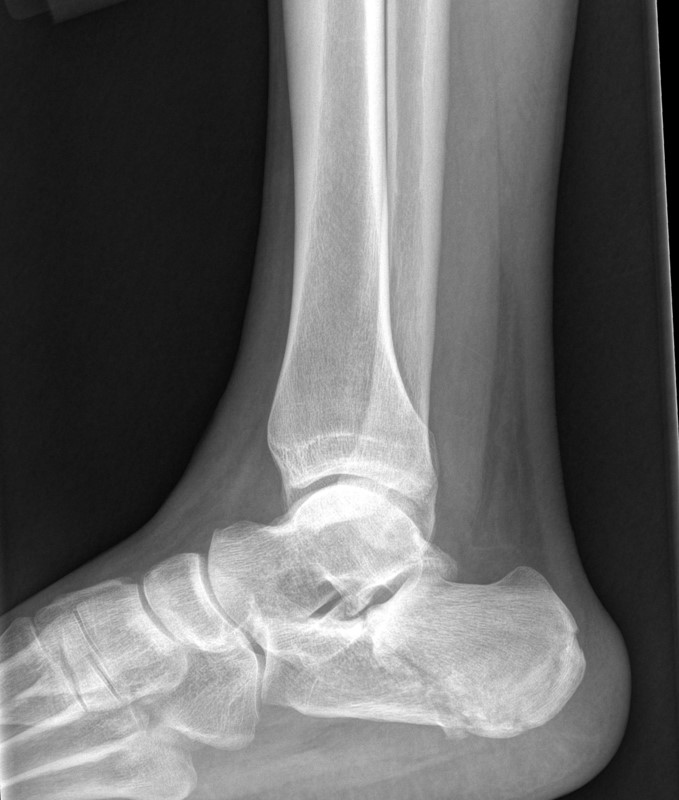
48 year-old presents after falling 15 feet following a “misunderstanding” with police. What's the diagnosis? ...and for a bonus question, why is this called a “Lover’s Fracture”?
Utility of Intra-Aortic Balloon Pump (IABP)
Compartment Syndrome
Compartment syndrome is classically described as having the 6 Ps:
The diagnosis of compartment syndrome can be difficult but ultimately it comes down to measuring the pressures in the area of concern. Various recommendations of the allowed pressure can be found, but in general a fasciotomy is not needed if the compartment pressure is 30 mmHg less then the diastolic pressure (The Delta 30). So if the patients diastolic pressure is 70, a fasciotomy is not need if the compartment pressure is less then 40.
Finally, if you are suspecting compartment pressure do NOT elevate the limb. Leave it in a dependent position to help improve blood flow into the limb.
Case: A 3 year 9 month female presents with fever to 39.4 C and intermittent abdominal pain worsening over 2 days. The patient had been tolerating food and had no change in her bowel habits. Based on the imaging below, what is your diagnosis and treatment?
All benzodiazepines are metabolized by the liver. Some are just metabolized by pathways that are less dependent on global liver function.
The ‘LOT’ drugs are metabolized by conjugation, have no active metabolites, and have minimially affected half-lives even in the setting of liver disease.
L – Lorazepam
O – Oxazepam
T – Temazepam
The rest of the benzodiazepines are primarily metabolized via hepatic CYP-mediated oxidation and may have prolonged duration of effect in patients with marked liver impairment.
For a bit more detail and commentary by Dr. David Juurlink, please read my recent post on the Academic Life in Emergency Medicine blog: http://academiclifeinem.com/all-benzodiazepines-are-metabolized-by-the-liver/
Helicopter EMS (HEMS) has rapidly grown over the past 30 years. HEMS is frequently used to transport trauma patients from the scene of a crash. The question is: for which trauma patients is HEMS most useful?
A recent article published in the Journal of the American Medical Association, based upon data from the National Trauma Data Bank (NTDB), looked at injured patients transported to a trauma center by helicopter versus ground ambulance. It showed that, after controlling for multiple known confounders, more severely injured patients had better outcomes when transported by helicopter than when transported by ground ambulances. Another recent article in the Journal of Trauma and Acute Care Surgery, again based upon the NTDB further showed that HEMS survival benefit seems to limited to individuals with physiologic instability.
Bottom Line:
Transport of severely injured trauma patients by helicopter versus ground from the scene of injury to a trauma center improved patient outcomes and decreased mortality. Transportation of stable, less injured patients by helicopter may actually worsen outcomes.
University of Maryland Section of Global Emergency Health
Author: Jon Mark Hirshon
Acalculous Cholecystitis in the Critically Ill
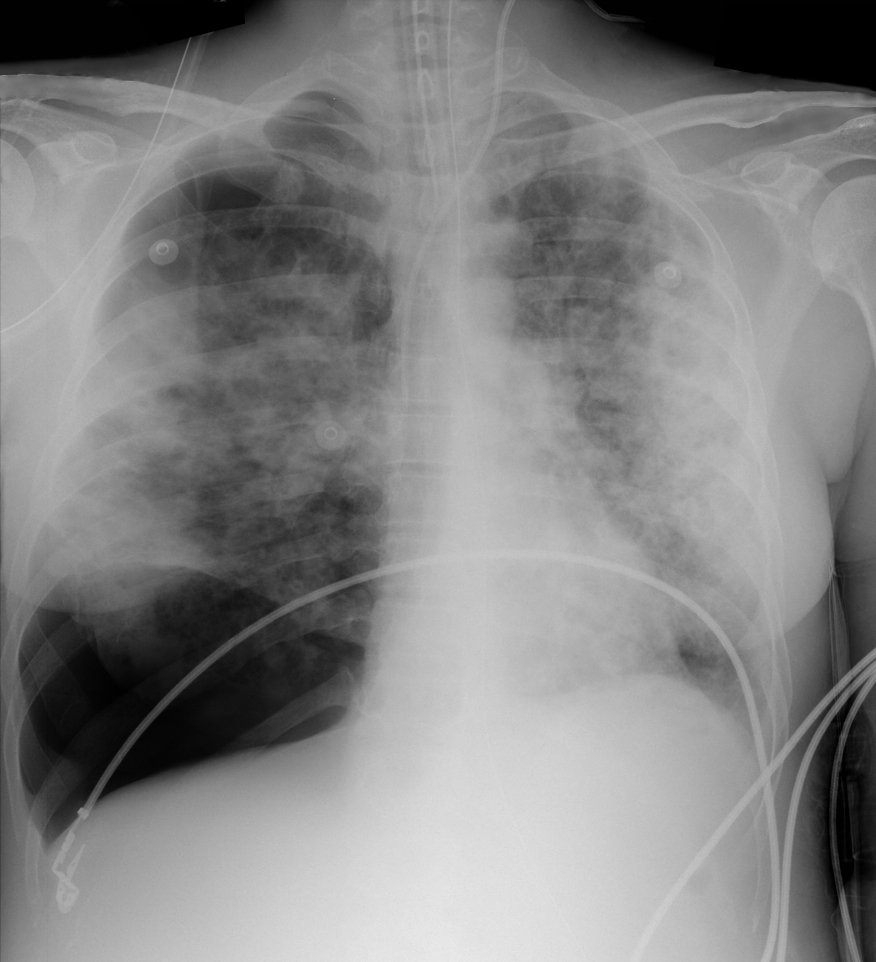
28 year-old cachectic female presents in respiratory distress and is immediately intubated on arrival to Emergency Department. What's the diagnosis and what are some potential etiologies?
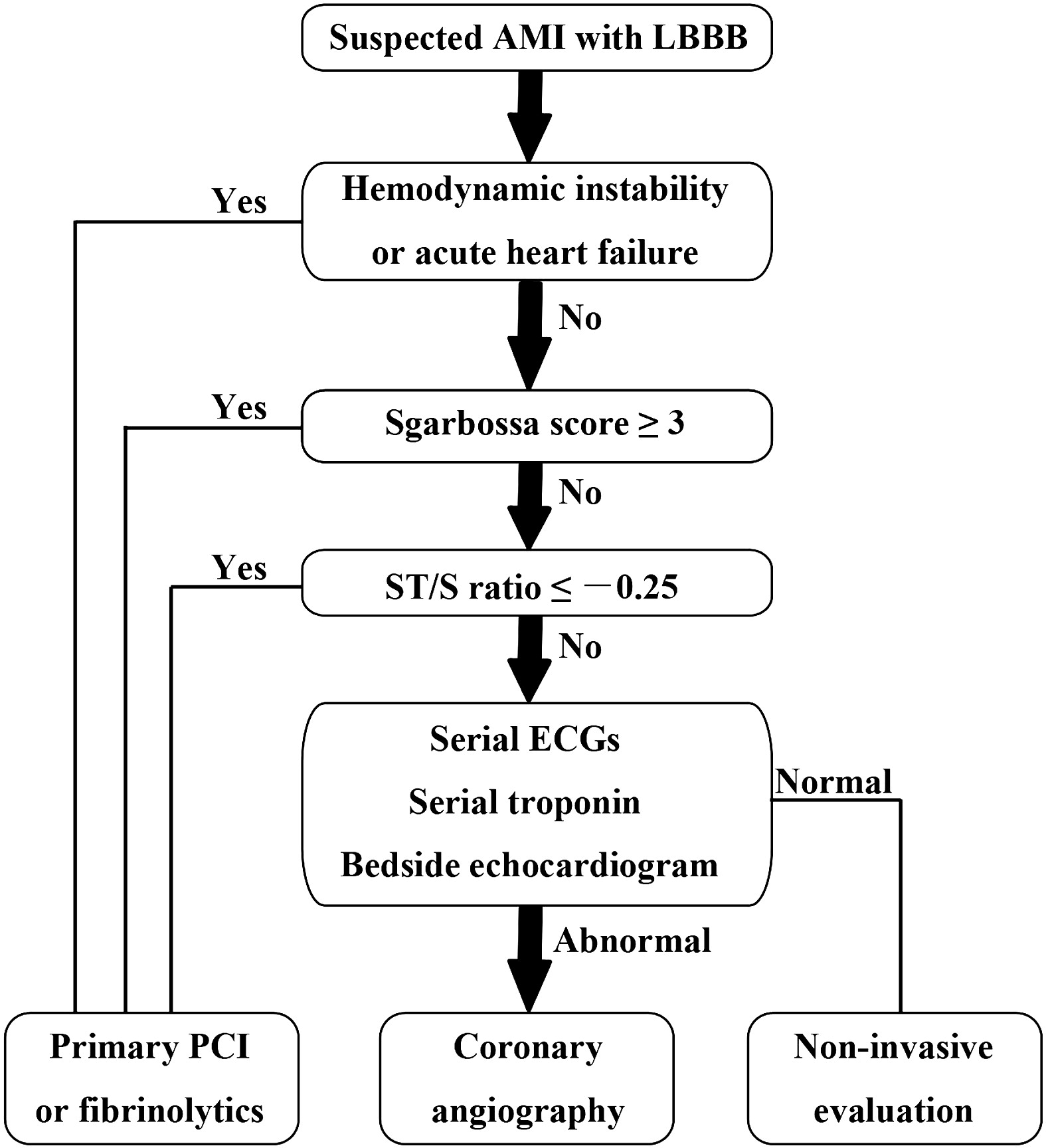
Diagnosis of STEMI in patients with LBBB can be challenging. Guidelines that previously recommended emergent reperfusion for these patients have been reconsidered to avoid inappropriate cath lab activation and fibrinolytic therapy.
The 2013 ACC/AHA STEMI guidelines no longer consider new or presumably new LBBB a STEMI equivalent. This dramatic change may prevent inappropriate therapy for some, but fail to help identify patients with LBBB who are having STEMI's. Delayed reperfusion in this population could be fatal and is estimated to affect 5,000-10,000 patients per year in the US alone.
The Sgarbossa ECG criteria are the most validated tool to aid in the diagnosis of STEMI in the presence of LBBB. A Sgarbossa score of ≥ 3 has high specificity (>98%) and positive predictive value for acute MI and angiography-confirmed coronary occlusion. The following algorithm has been recently proposed to identify the high-risk population in which reperfusion therapy would be denied by the 2013 STEMI guidelines.
Watch this video to review Sgarbossa criteria and the modified Sgarbossa rule.
Want more emergency cardiology pearls? Follow me @alifarzadmd
Cauda equina syndrome results from compression of multiple lumbar and sacral nerve roots
Causes: Central disc herniation, spinal epidural abscess, malignancy, trauma, hematoma.
Consider this entity in those with back pain and radiculopathy at multiple spinal levels
Urinary retention occurs in >90% of patients
Saddle anesthesia occurs in 75%
Decreased rectal sphincter tone occurs in 60 to 80%
A post void residual volume <100 mL makes this entity very unlikely
When patients with severe allergies to penicillin (urticarial, bronchospasm, anaphylaxis, angioedema) are excluded, the cross reactivity to cephalosporins is very low (approximately 0.1%)
The reaction is related to structures in the side chain, not the cyclical structure as thought in the past.
There are several cephalosporins with IDENTICAL side chains that should not be given to patients with allergies to specific penicillins, namely: