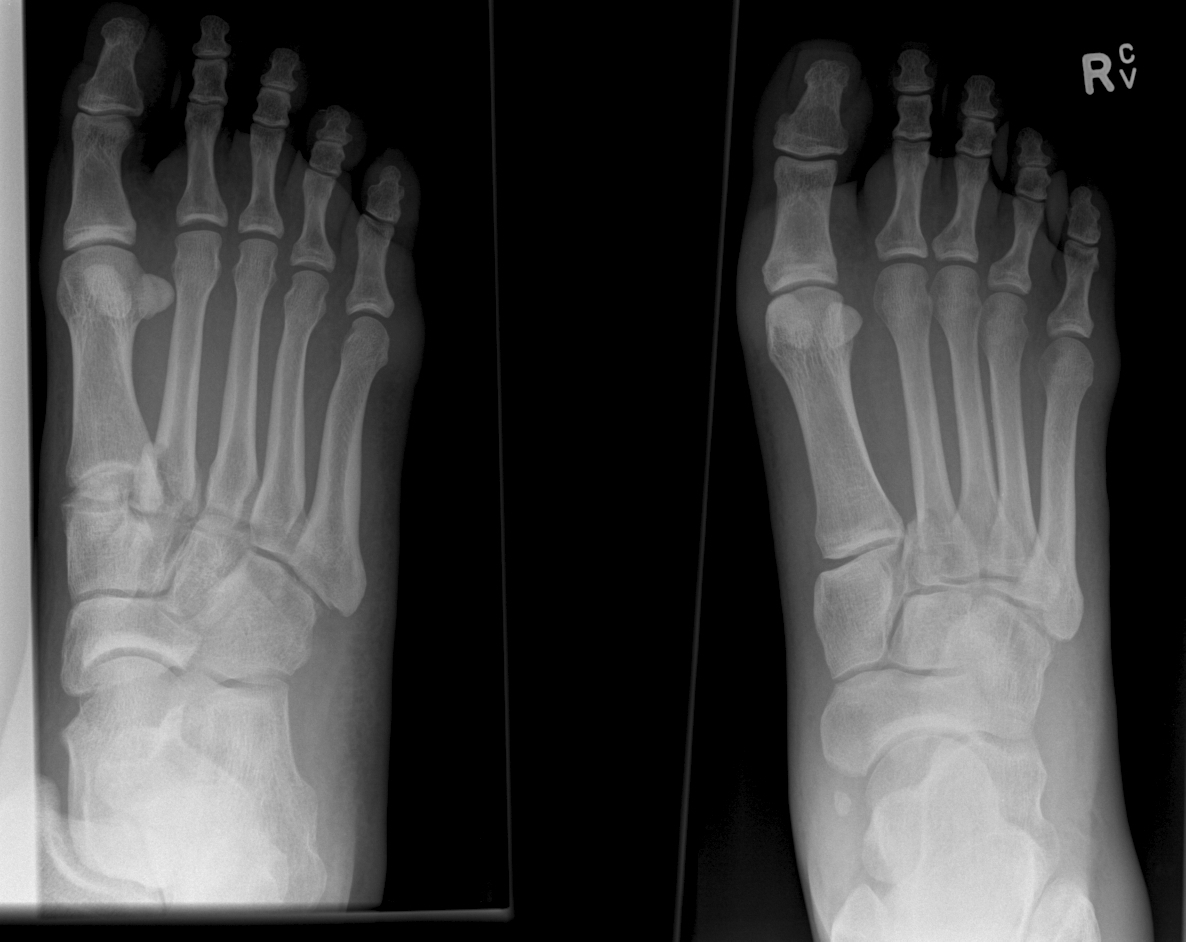
Lisfranc Fracture:
Typically consists of a fracture of the base of the second metatarsal and dislocation, though it can also be associated with fractures of a cuboid. Common current mechanism of injury is when a person steps into a hole and twists the foot. The original mechanism of injury that was described was when a horseman would fall of their horse with their foot still trapped in a stirrup.
Diagnosis should be considered if patient has difficultly weight bearing with pain on palpation over the 2nd and 3rd metacarpal head with an appropriate mechanism.
Pearls:
- Fracture findings on plain films may be subtle.
- If in doubt obtain weight bearing AP views of the foot to demonstrate dislocation/fracture.
- If weight bearing films are negative and you are still suspicious consider a CT scan of the foot.