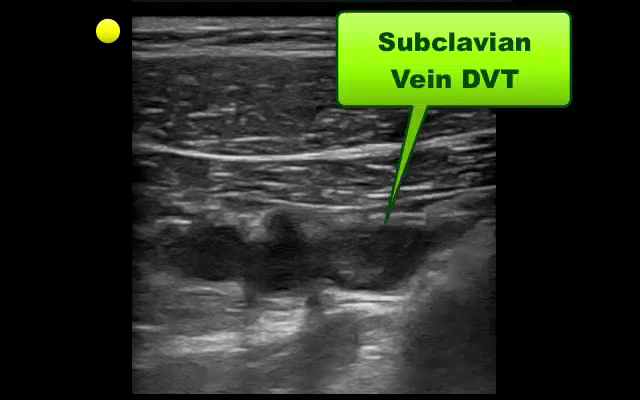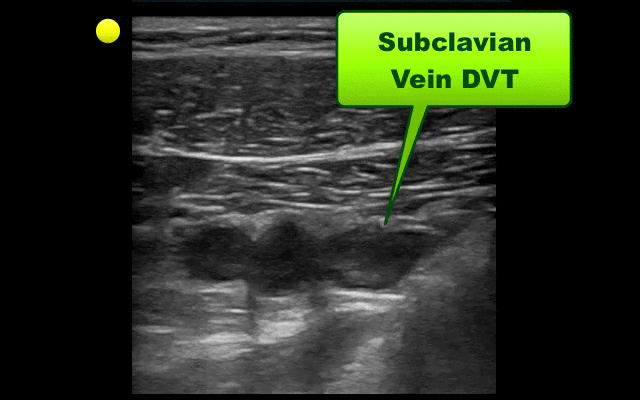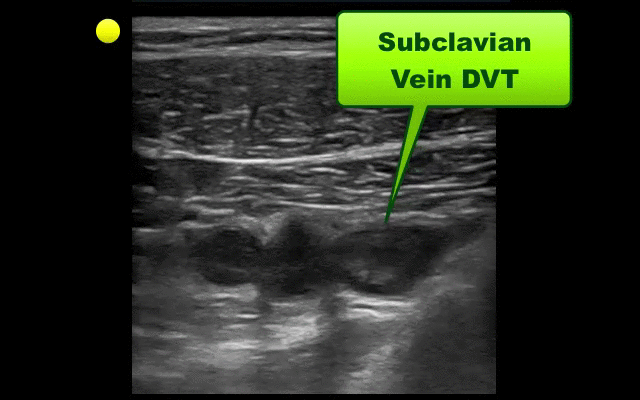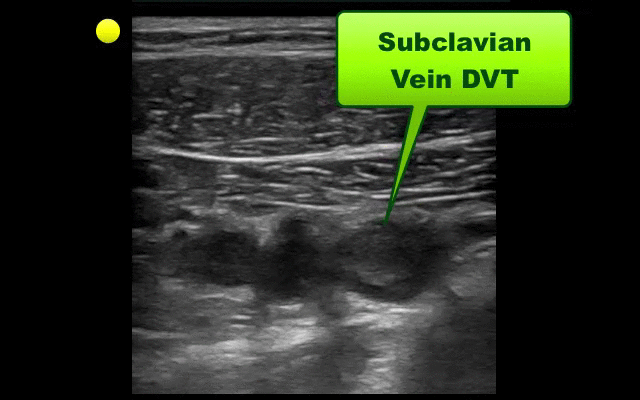
UEDVT comprise 10% of all DVTs (majority are lower extremity), but incidence of UEDVT is rising; UEDVTs are categorized into distal (veins distal to axillary vein) or proximal (from superior vena cava to axillary vein)
Compared to lower extremity DVT, UEDVTs have lower:
- mortality
- risk of pulmonary embolism
- rates of recurrence
75% of UEDVT are secondary (indwelling catheters, pacemakers, malignancy, etc.) and 25% are primary in nature; #1 primary cause of UEDVT is Paget – Schroetter disease
Up to 25% of patients with primary UEDVTs are eventually found to have an underlying malignancy; patients with idiopathic UEDVT should be referred for cancer workup
Treatment includes removal of the catheter (if no longer needed) and:
- anticoagulation (minimum of 3 months)
- consideration of thrombolytics, including catheter-directed administration
- mechanical thrombolysis (clot aspiration, fragmentation, etc.)
- surgical thrombectomy / venous bypass