Question
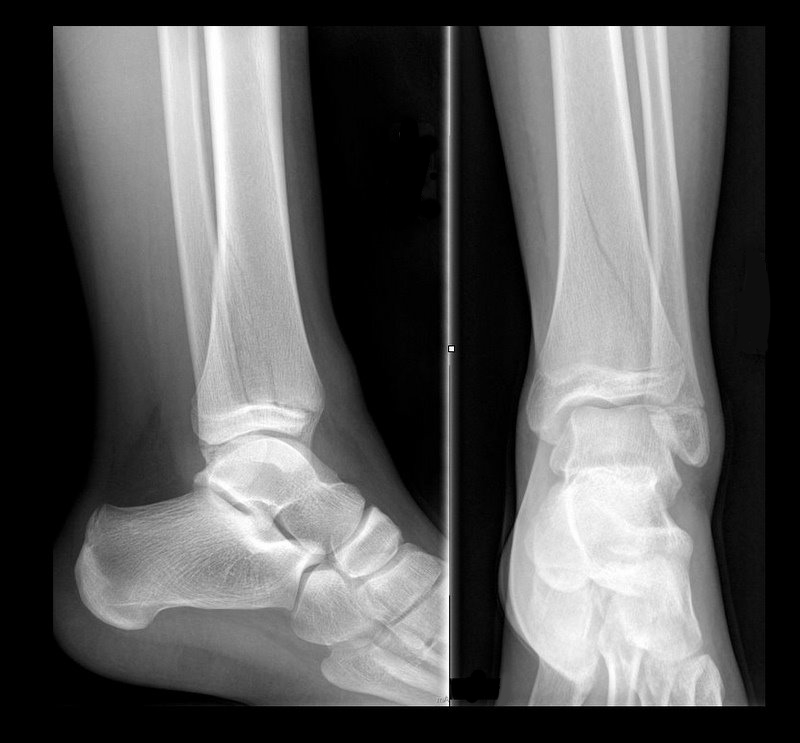
13 year-old female with ankle pain following fall down escalator. What's the diagnosis?
Keep Immune Thrombocytopenic Purpura (ITP) in your differential for patients with thrombocytopenia and evidence of bleeding. Although ITP has classically been described in children, it can occur in adults; especially between 3rd- 4th decade.
Thrombocytopenia leads to the extravasation of blood from capillaries, leading to skin bruising, mucus membrane petechial bleeding, and intracranial hemorrhage.
ITP occurs from production of auto-antibodies which bind to circulating platelets. This leads to irreversible uptake by macrophages in the spleen. Causes of antibody production include:
Suspect ITP in patients with isolated thrombocytopenia on a CBC without other blood-line abnormalities. Abnormality in other blood-line warrants consideration of another diagnosis (e.g., leukemia).
ITP cannot be cured; treatments include:
13 year-old female with ankle pain following fall down escalator. What's the diagnosis?

Therapeutic hypothermia (TH) following out-of-hospital cardiac arrest (OHCA) has increasingly been utilized since it was first described. TH following in-hospital cardiac arrest (IHCA), on the other hand, is not as commonplace or consistent despite a recommendation by the American Heart Association (AHA).
A recent prospective multi-center cohort-study demonstrated that of 67,498 patients with return of spontaneous circulation (ROSC) following IHCA only 2.0% of patients had TH initiated; of those 44.3% did not even achieve the target temperature (32-34 Celsius).
The factors found to be most associated with instituting TH were:
Bottom-line: Hospitals should consider instituting and adhering to local TH protocols for in-house cardiac arrests.
Ever wonder how to place a pigtail catheter?
Check out this video to learn how, click here
9 month-old presents with wheezing and the CXR is shown below. What's the diagnosis?
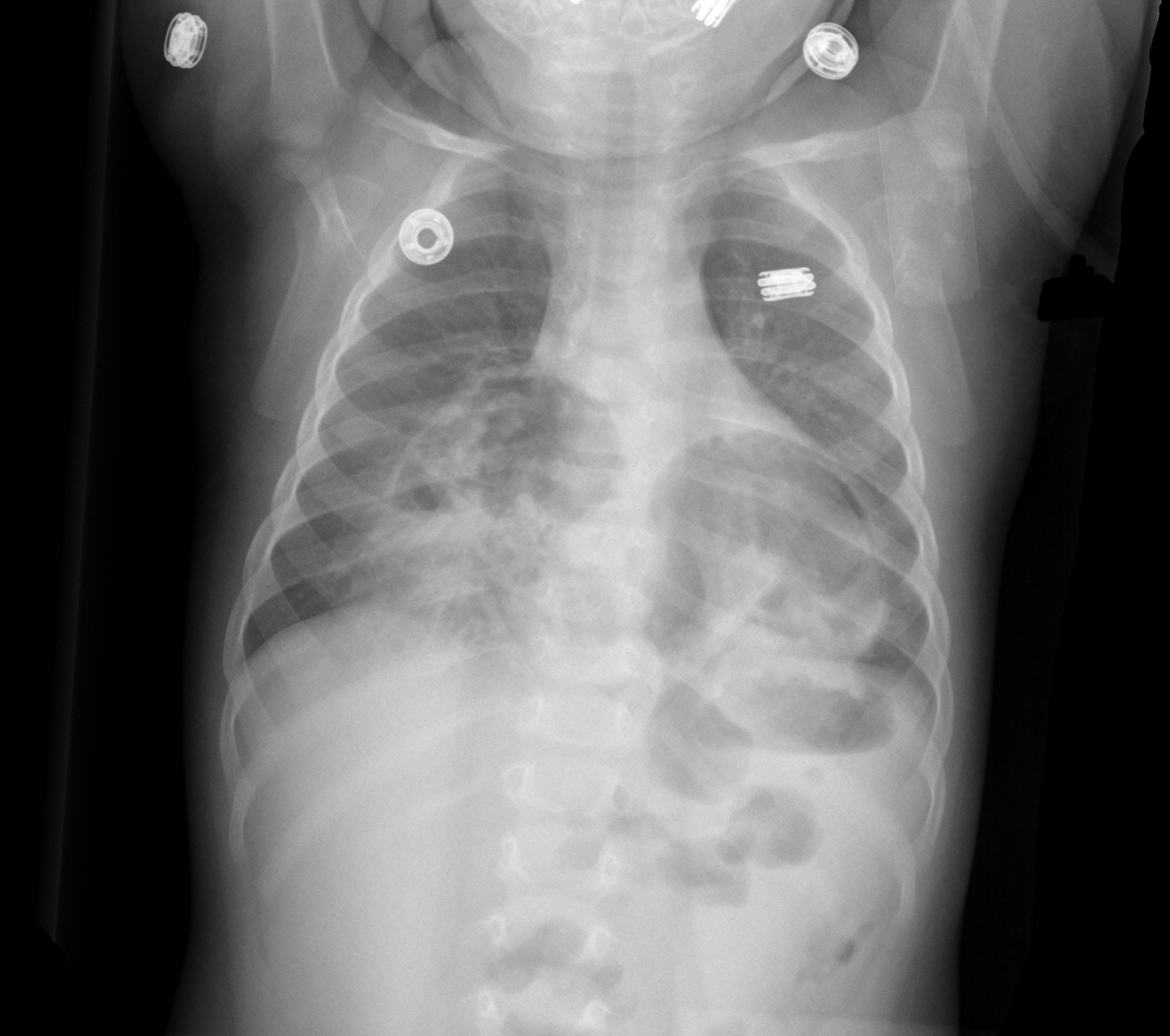
The Macklin Effect
Pneumomediastinum (click here for image) may be caused by many things:
The "Macklin Effect" is typically a self-limiting condition leading to spontaneous pneumomediastinum and massive subcutaneous emphysema after the following:
Pneumomediastinum secondary to the Macklin effect frequently leads to an extensive workup to search for other causes of mediastinal air. Although, no consensus exists regarding the appropriate workup, the patient's history should guide the workup to avoid unnecessary imaging, needless dietary restriction, unjustified antibiotic administration, and prolonged hospitalization.
Treatment of spontaneous pneumomediastinum includes:
30 year-old male presents with right wrist pain after falling off his bicycle. What's the diagnosis?
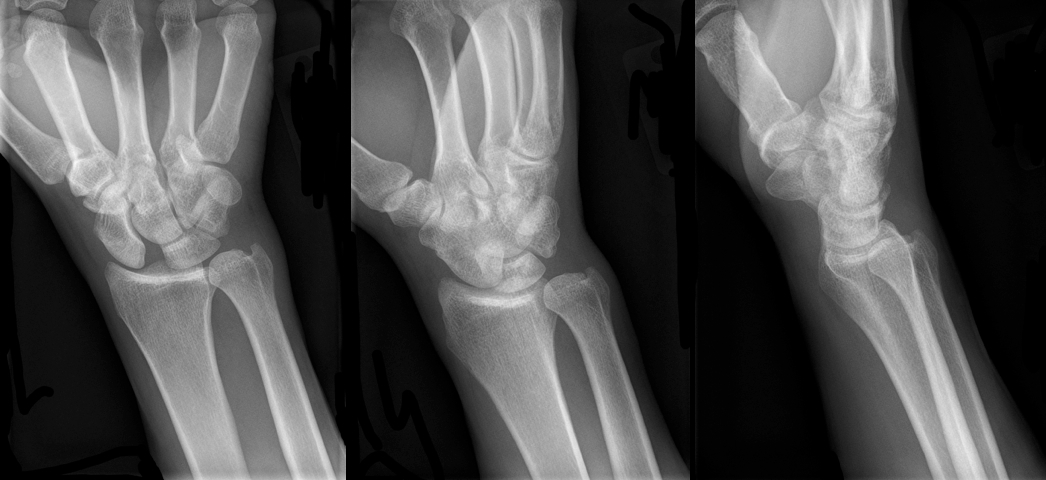
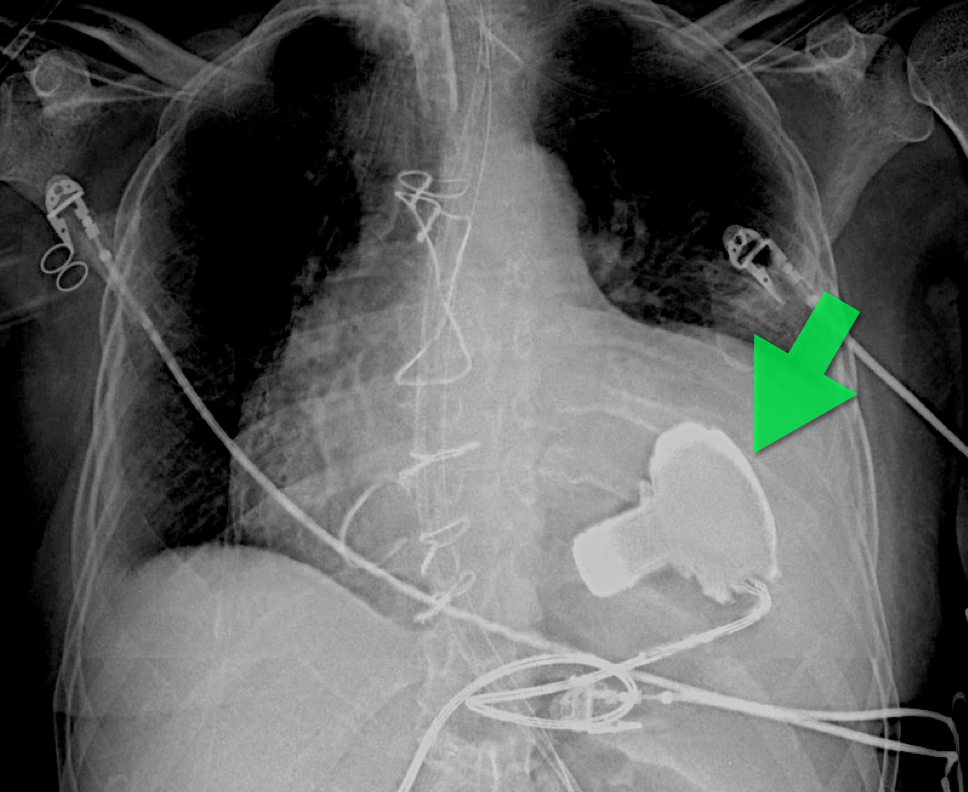
60 year-old male with a history of pulmonary fibrosis presents to the Emergency Department after a lung biopsy. He is complaining of facial swelling and dyspnea. What's the diagnosis?
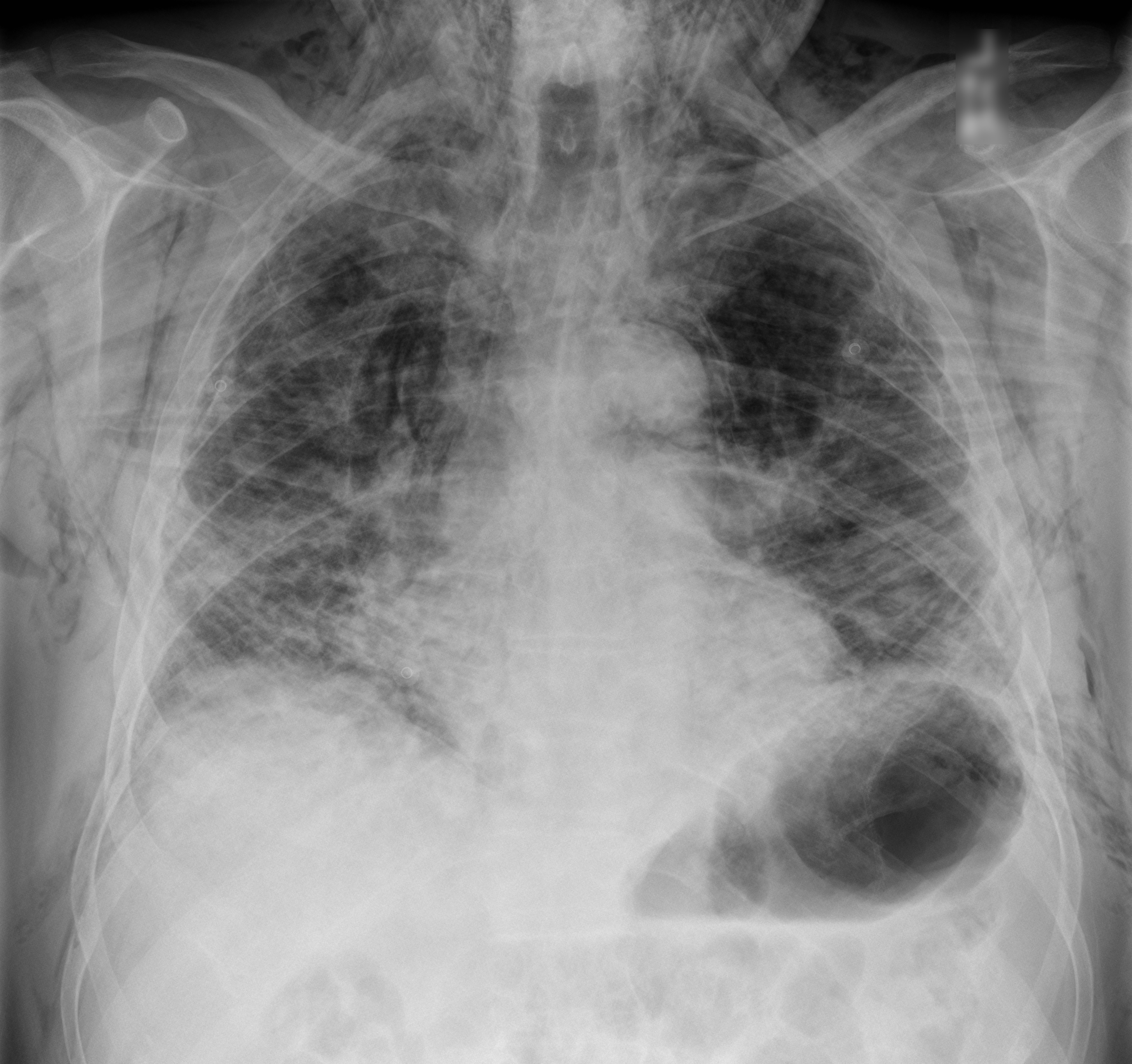
Fluid boluses are often administered to patients in shock as a first-line intervention to increase cardiac output. Previous literature states, however, that only 50% of patients in shock will respond to a fluid bolus.
Several validated techniques exist to distinguish which patients will respond to a fluid bolus and which will not; one method is the passive leg raise (PLR) maneuver (more on PLR here). A drawback to PLR is that it requires direct measurement of cardiac output, either by invasive hemodynamic monitoring or using advanced bedside ultrasound techniques.
Another technique to quantify changes in cardiac output is through measurement of end-tidal CO2 (ETCO2). The benefits of measuring ETCO2 is that it can be continuously measured and can be performed non-invasively on mechanically ventilated patients.
A 5% or greater increase in end-tidal CO2 (ETCO2) following a PLR maneuver has been found to be a good predictor of fluid responsiveness with reliability similar to invasive measures.
38 year-old male with a past medical history of diabetes presents with back pain and hypotension. CT scan is shown below. What's the diagnosis?
57 year old male presents with a cough. The CXR is shown below. What's the diagnosis?
Necrotizing fasciitis (NF) is a rapidly progressive bacterial infection of the fascia with secondary necrosis of the subcutaneous tissue. In severe cases, the underlying muscle (i.e., myositis) may be affected.
Risk factors for NF include immunosuppression (e.g., transplant patients), HIV/AIDS, diabetes, etc.
There are three categories of NF:
In the early stage of disease, diagnosis may be difficult; the physical exam sometimes does not reflect the severity of disease. Labs may be non-specific, but CT or MRI is important to diagnose and define the extent of the disease when planning surgical debridement.
Treatment should be aggressive and started as soon as the disease is suspected; this includes:
35 year-old female presents with fever and hypotension. Bedside ultrasound is performed and is shown here. What's the diagnosis?
Adrenal insufficiency (AI) can be a life-threating condition and is classified as primary (failure of the adrenal gland) or secondary (failure of hypothalamic- pituitary axis).
Common causes of primary adrenal insufficiency include autoimmune destruction, infectious causes (TB and CMV), or interactions with drugs (e.g., anti-fungals, Etomidate, etc.). Secondary causes are usually due to abrupt withdrawal of steroids after chronic use, although sepsis and diseases of the hypothalamus or pituitary (e.g., CVA) may occur.
Signs and symptoms include fatigue, weakness, skin pigmentation, dizziness, abdominal pain, and orthostatic hypotension; it should be suspected with any of the following: hyponatremia, hyperkalemia, hypoglycemia, hypercalcemia, low free-cortisol level, and hemodynamic instability despite resuscitation.
Treatment:
• Correct underlying the disorder
• Resuscitation and hemodynamic support
• Correct hypoglycemia and electrolyte abnormalities
• Treat with hydrocortisone, cortisone, prednisone, or dexamethasone +/- fludrocortisone (Note: dexamethasone is attractive choice in the ED because it will not interfere with ACTH stimulation test)
64 year-old female presents with chest pain following an argument with her husband. Her echocardiogram (apical four-chamber view) and ECG are shown. Her initial troponin is 10. What's the diagnosis?

There are several reasons why a mechanically ventilated patient may decompensate post-intubation. Immediate action is often needed to reverse the problem, but it can be difficult to remember where to start as the vent alarm is sounding and the patient is decompensating.
Consider using the mnemonic “D.O.P.E.S. like D.O.T.T.S.” to assist you in first diagnosing the problem (D.O.P.E.S.) and then fixing the problem (D.O.T.T.S.). You can view an entire lecture on the Crashing Ventilated Patient here.
Step 1: Could this decompensation be secondary to D.O.P.E.S.?
Step 2: Fix the problem with D.O.T.T.S.
35 year-old male presents after a motor vehicle crash. No blood seen at the meatus of the penis and a Foley catheter is placed (see photo below). What's the next diagnostic step?

A 56-year-old woman with a history of psoriasis presents with fever, nausea, and painful pin-point pustules on an erythematous base. Her dermatologist recently reduced her prednisone dose. What's the diagnosis?

Mechanically ventilated patients can develop a condition in which air becomes trapped within the alveoli at end-expiration; this is called auto-PEEP.
Auto-peep has several adverse effects:
Auto-PEEP classically occurs in intubated patients with asthma or emphysema, but it may also occur in the absence of such disease. The risk of auto-PEEP is increased in patients with:
Auto-PEEP may be treated by:
Patients may need to be heavily sedated to accomplish the above ventilator maneuvers.