Question
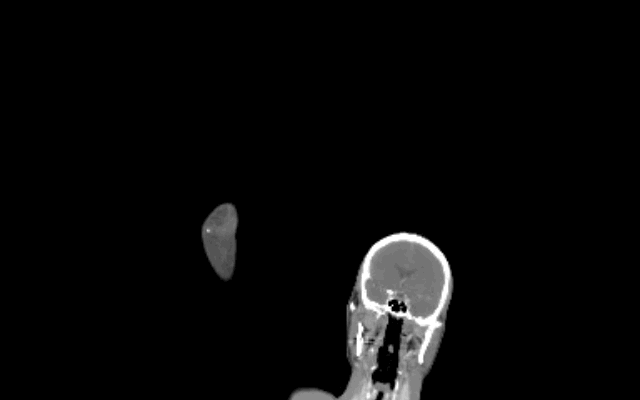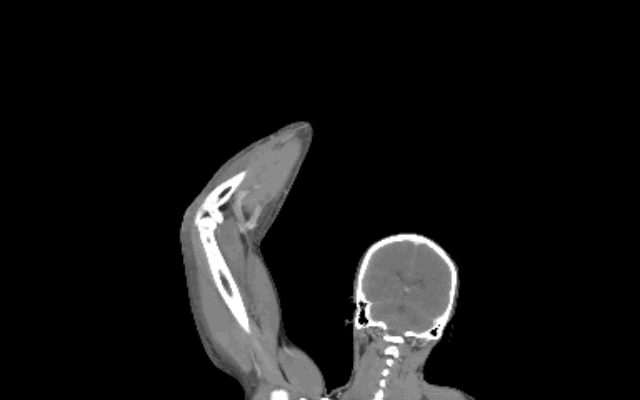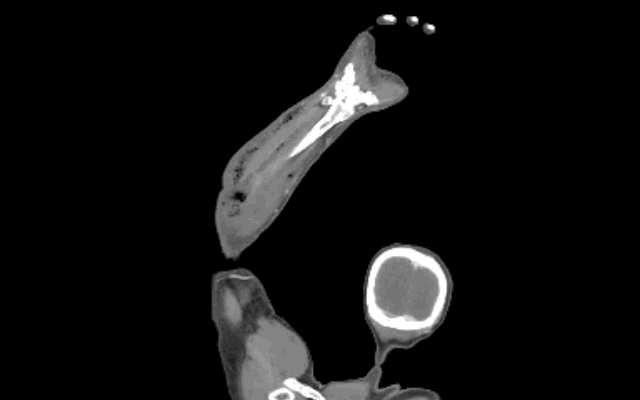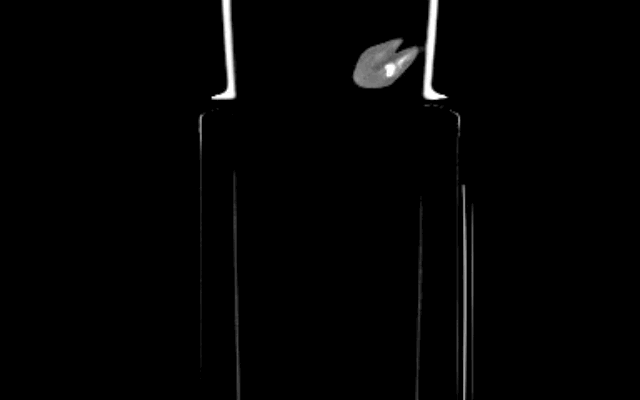
CXR shown below, what's the diagnosis? ...and name 3 differential diagnoses.
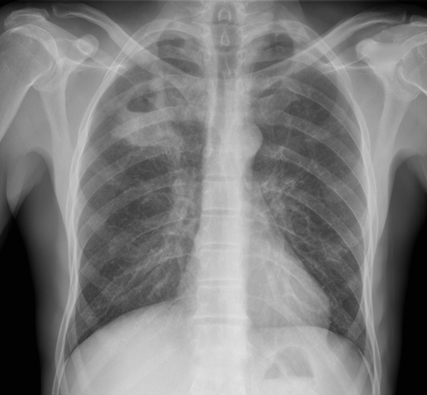
CXR shown below, what's the diagnosis? ...and name 3 differential diagnoses.

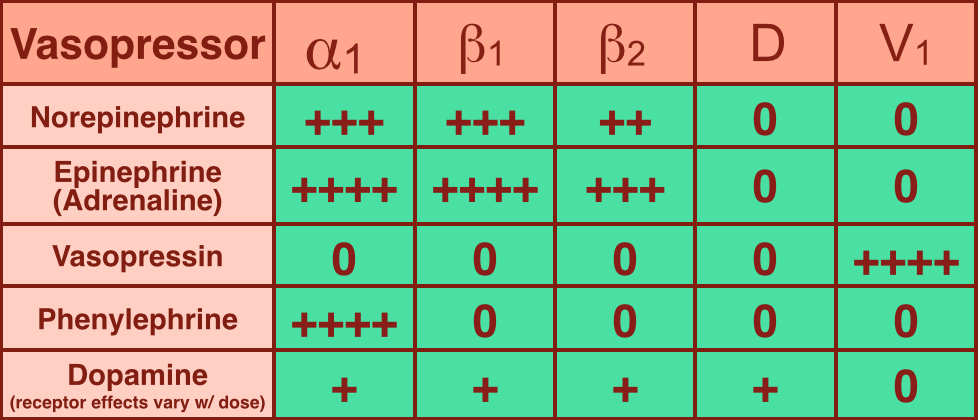
Vasopressors are used in shock-states to increase mean arterial pressure (MAP) and improve distal tissue perfusion. Additionally, some agents have effects on the heart to augment cardiac output.
Receptors that vasopressors work on include:
Norepinephrine (NE): excellent vasopressor for most types of shock and recommended as a first-line agent in the Surviving Sepsis Guidelines.
Epinephrine (a.k.a. Adrenaline): in several countries the first-line agent for shock (including sepsis).
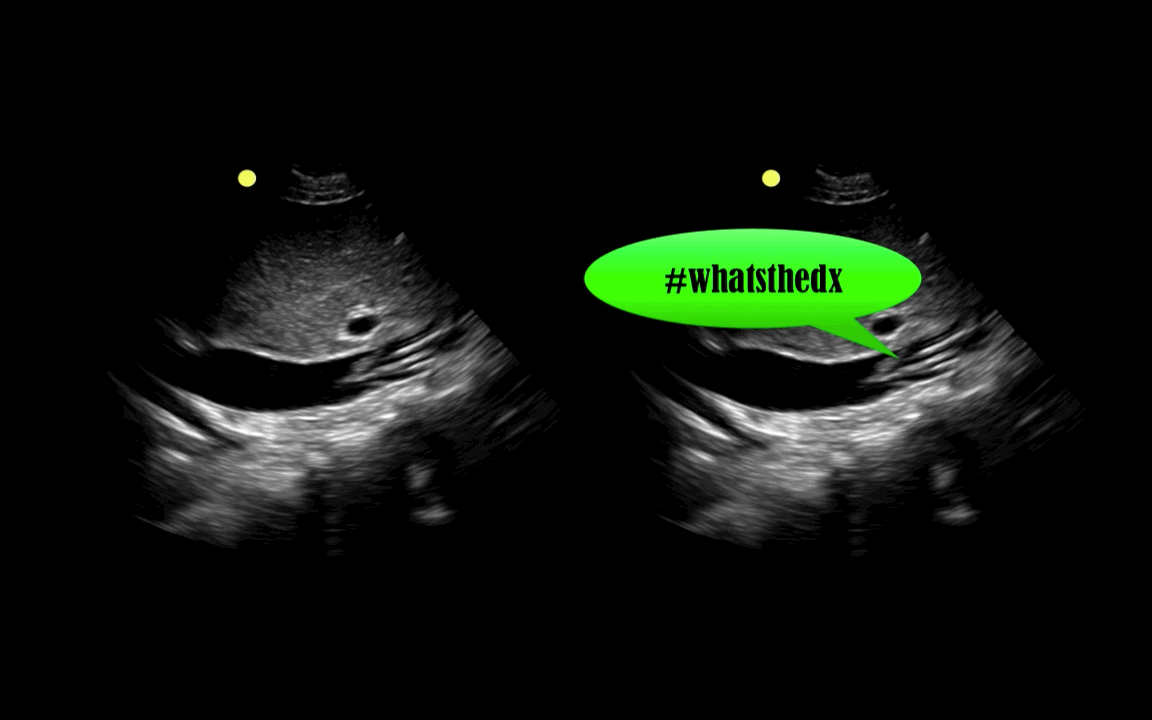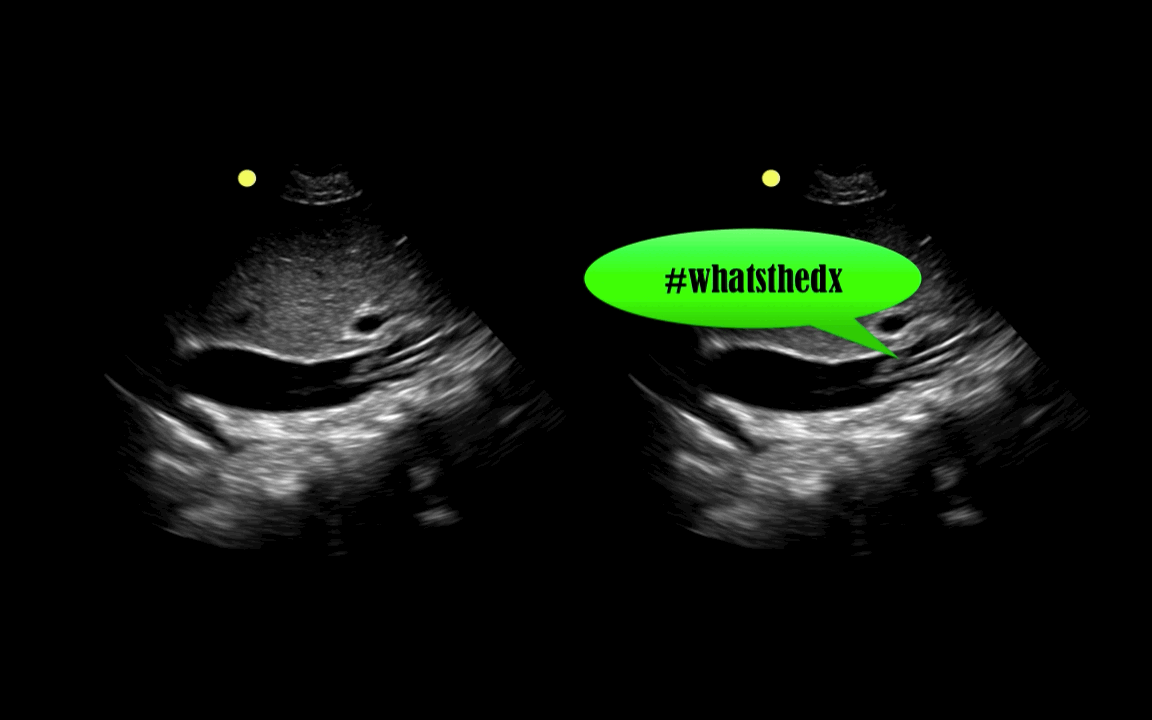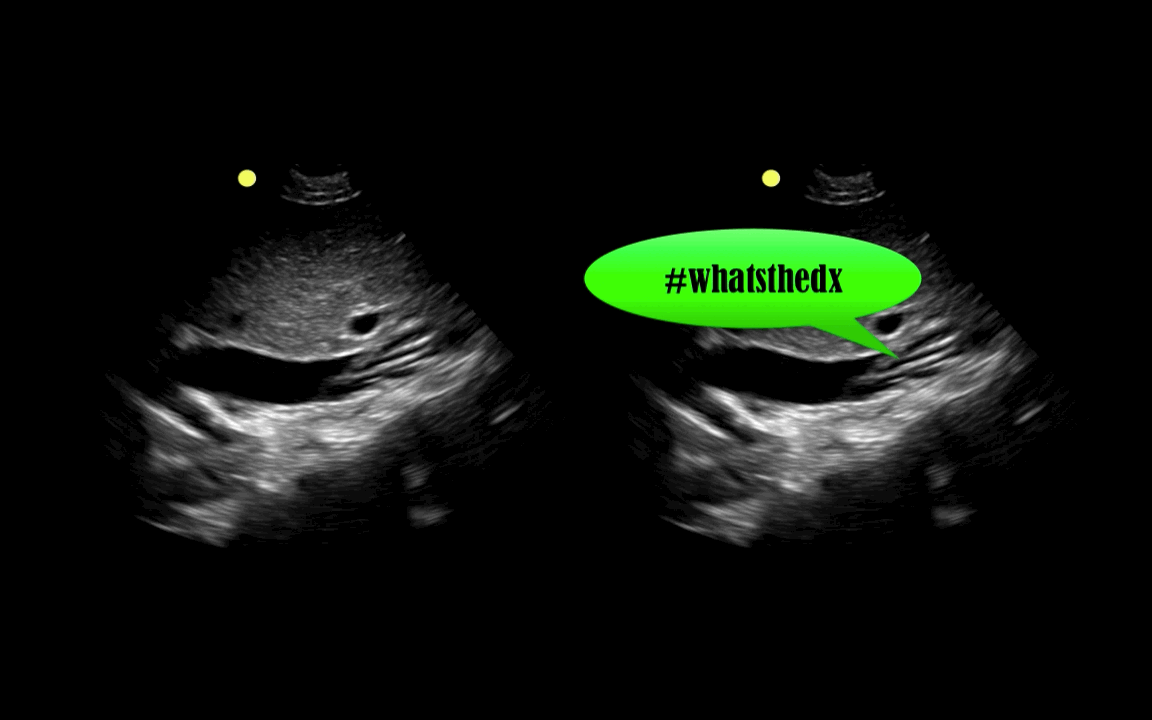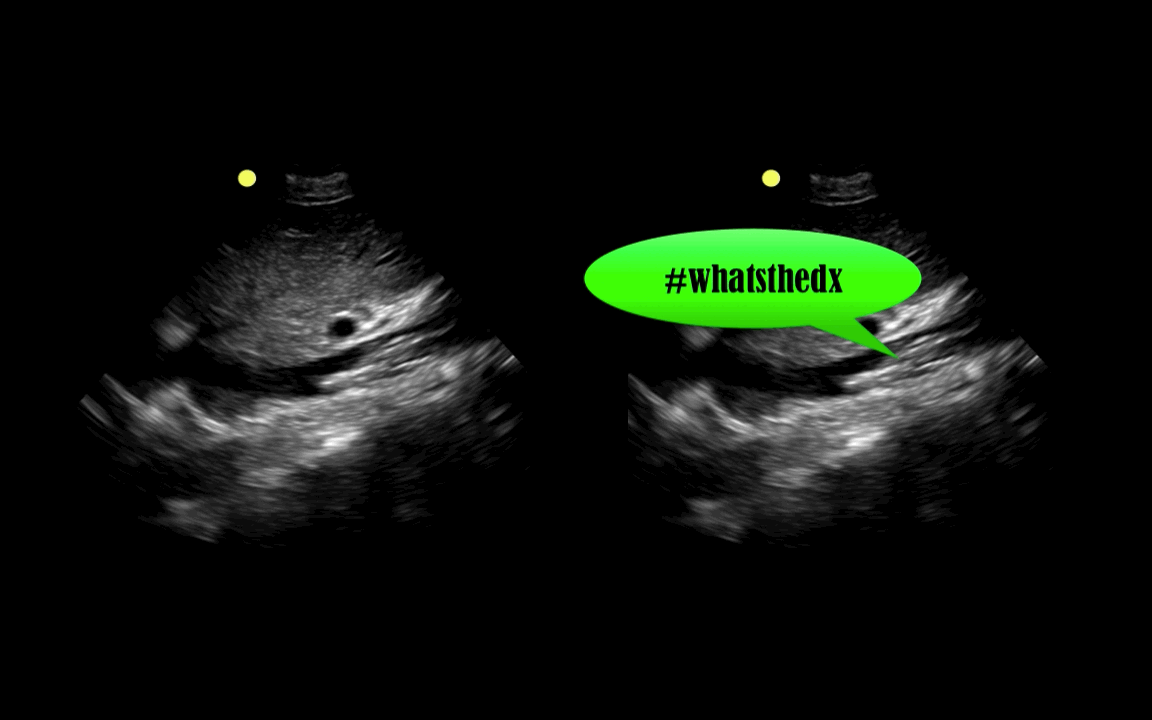
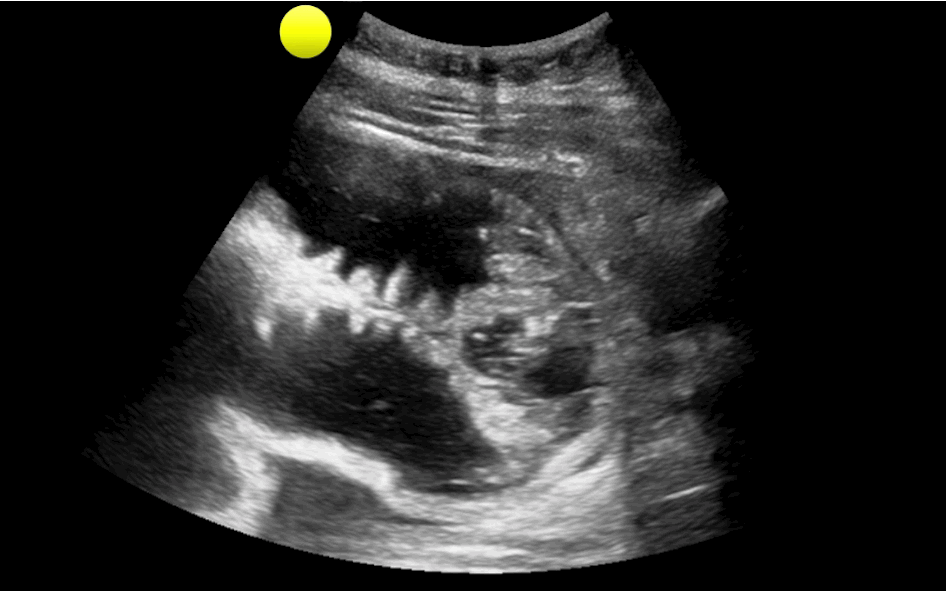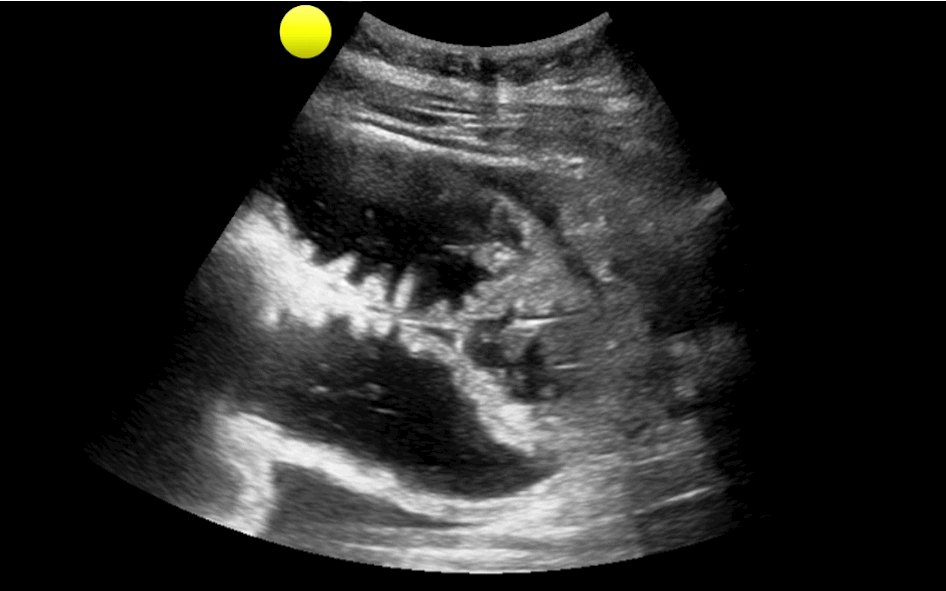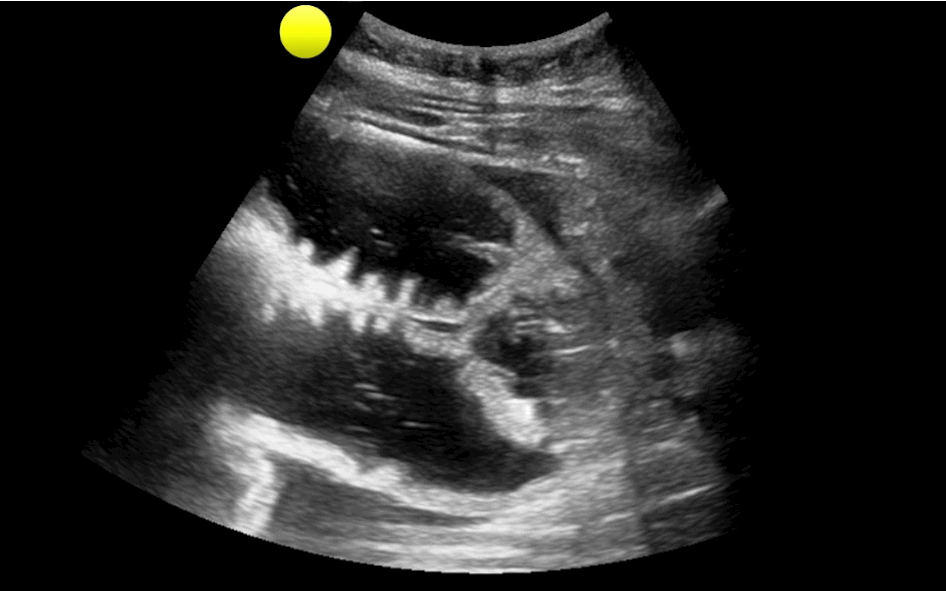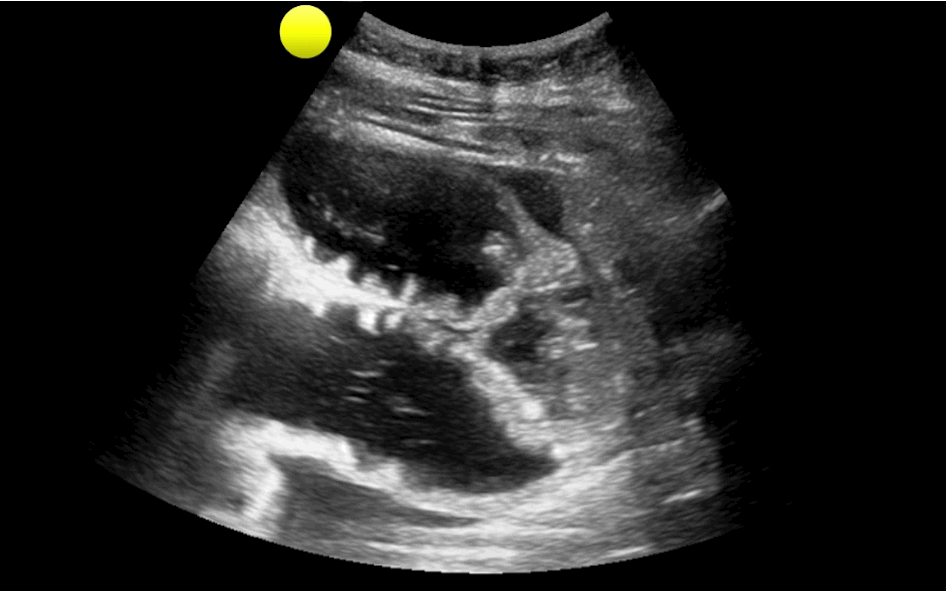
You are scaning the liver with ultrasound and you see this. What's the diagnosis?
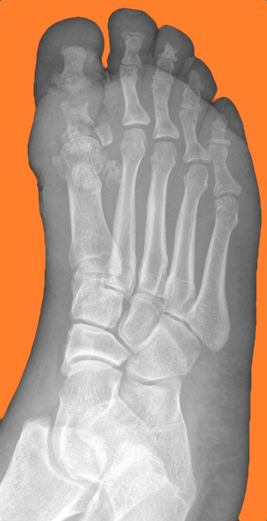
50 year-old female with diabetes complains of pain and discharge from a poorly healing wound. XRay below. What's the diagnosis?
A critically-ill patient requires fluid resuscitation. Someone hands you a bag of this. What’s the pH of this fluid?

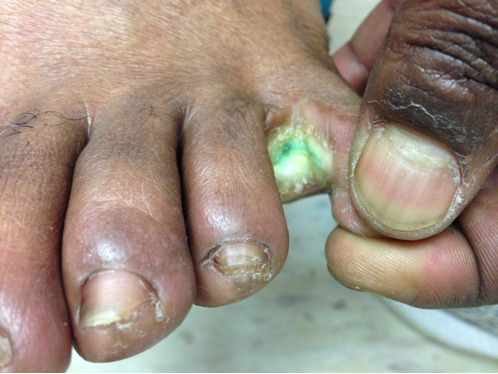
30 year-old female with complains of night sweats and painful lesions on her fingertips. What’s the diagnosis and list some things to have in the differential diagnosis?

There are many ventilator modes to choose from, but almost every mode can be distilled down to its basic principles by understanding the “Three T's of Mechanical Ventilation”
Trigger: You must determine whether the vent or patient will trigger a mechanical breath. For example, machine-triggered breaths (a.k.a. control mode of ventilation) are used for paralyzed patients and will deliver a breath after a period of time has elapsed (e.g., if RR is 10/min, then a breath is given every 6 seconds). On the other hand, if a patient’s respiratory drive is intact (a.k.a. assist-mode) than the patient triggers the breath when the vent detects a patient induced change in airflow or airway pressure. These two modes can also be mixed together.
Target: Mechanical breaths must have a specific target, either a target airway pressure or a tidal volume. Because pressure and volume are directly related, pick the variable you want to target and the other parameter will vary depending on the patient’s intrinsic physiology. For example, if you choose to target a specific tidal volume, we may get one plateau pressure in a patient with normal lungs, but a higher plateau pressure in another patient with stiffer lungs.
Terminate: You must decide when the mechanical breath (i.e., inspiration) terminates and expiration begins. Termination occurs: 1) after a set inspiratory time has elapsed in certain pressure-targeted modes, 2) when a predefined target volume has been achieved (i.e., volume-cycled modes), or 3) when airflow has been reduced by a certain percentage (as in pressure-support ventilation; to be discussed separately)
Let’s put this all together by looking at an example: pressure control ventilation (rate = 12/min and target pressure 20cm H20). Trigger: Because this is a “control”, not assist mode, the machine will trigger a breath 12 times per minute or every 5 seconds. Target: Here we chose to have pressure be the target, so when the ventilator triggers a breath it will deliver a constant airway pressure of 20 cmH2O until we tell the vent terminate that breath. Terminate: the constant airway pressure will be turned off after a fixed period of time has elapsed; for this example we will set the inspiratory time as 1 second, then expiration begins. Now, after a few vent breaths we will observe the results of our settings and reassess; if the resulting tidal volume is lower than what we wanted, we will increase the target pressure to increase the tidal volume. If the tidal volume is higher than what we wanted, we will reduce the target pressure to reduce the tidal volume. We can also tweak the inspiratory time to manipulate the tidal volume, but this does so to a lesser degree.
Try to break down your favorite modes of ventilation using the Three T’s and see if this helps you understand vent modes better.
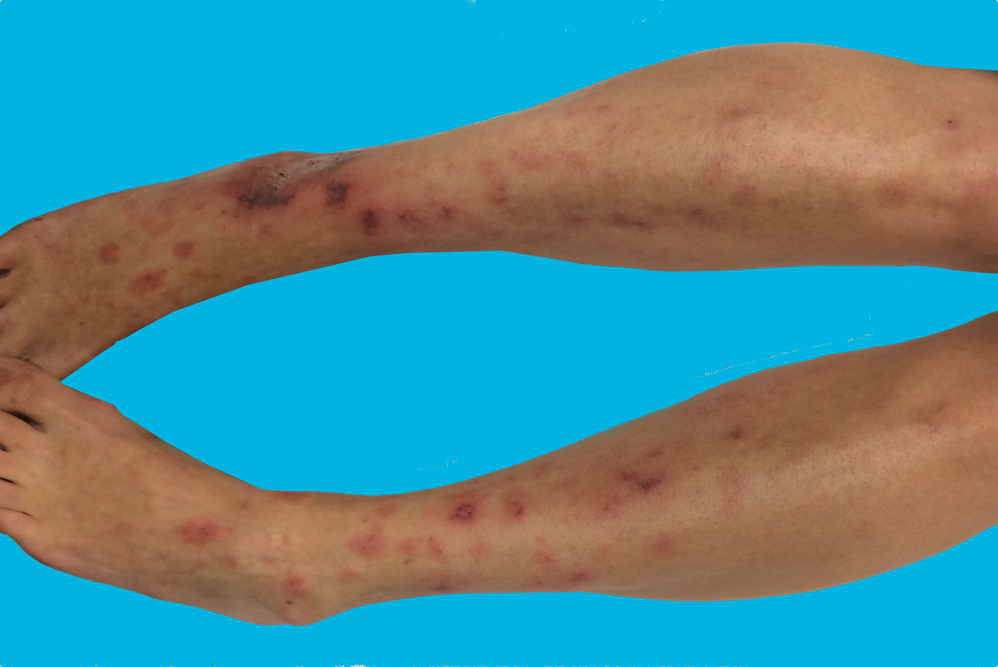
40 year-old female presents with painful lesions and ulcers on lower extremities. She has had this before, but never to this extent. She also has a history of DVT. What’s the diagnosis?
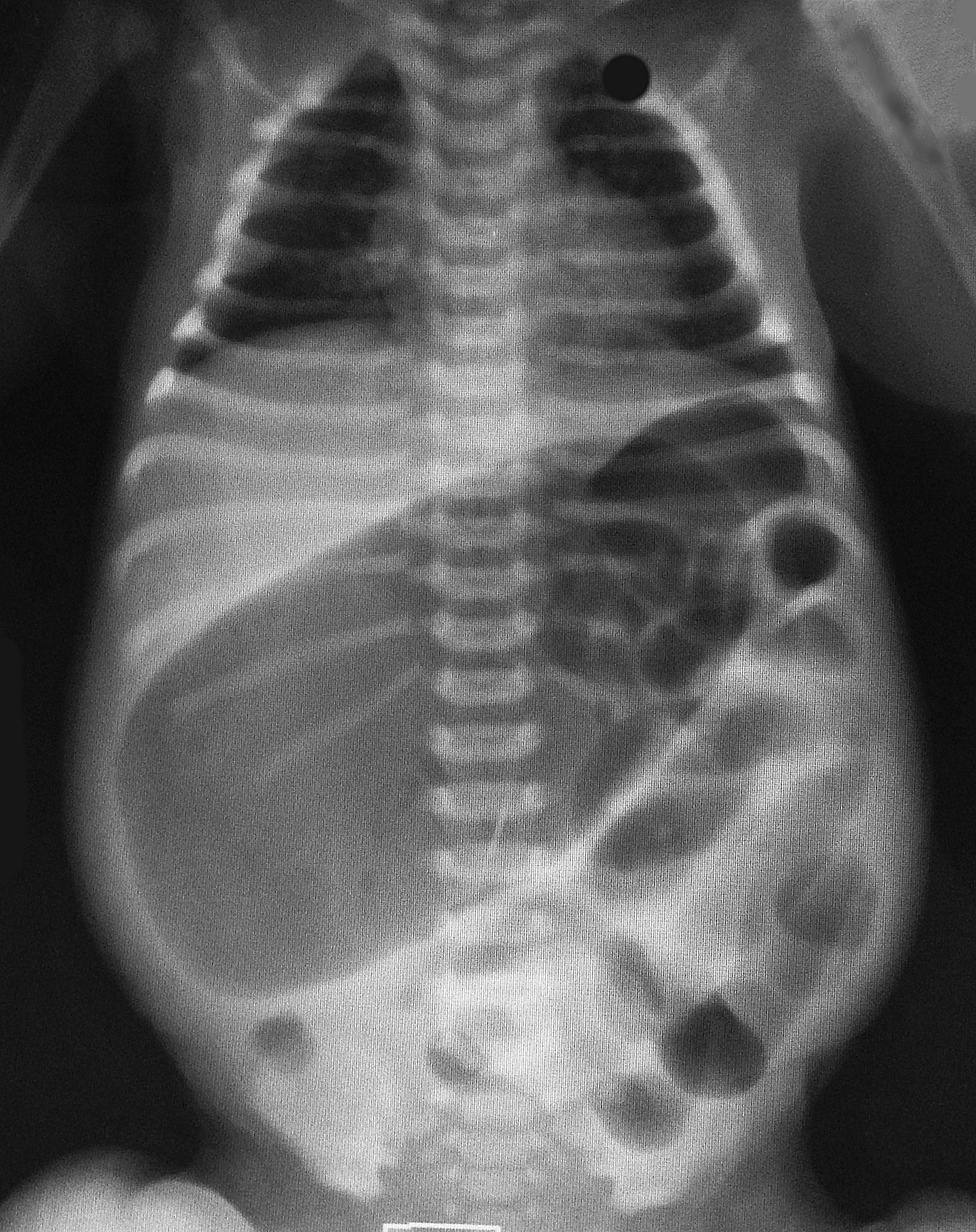
2-day old baby boy presents with forceful vomiting of entire feeds, bloated belly, and has not passed stools since birth. What's the diagnosis?
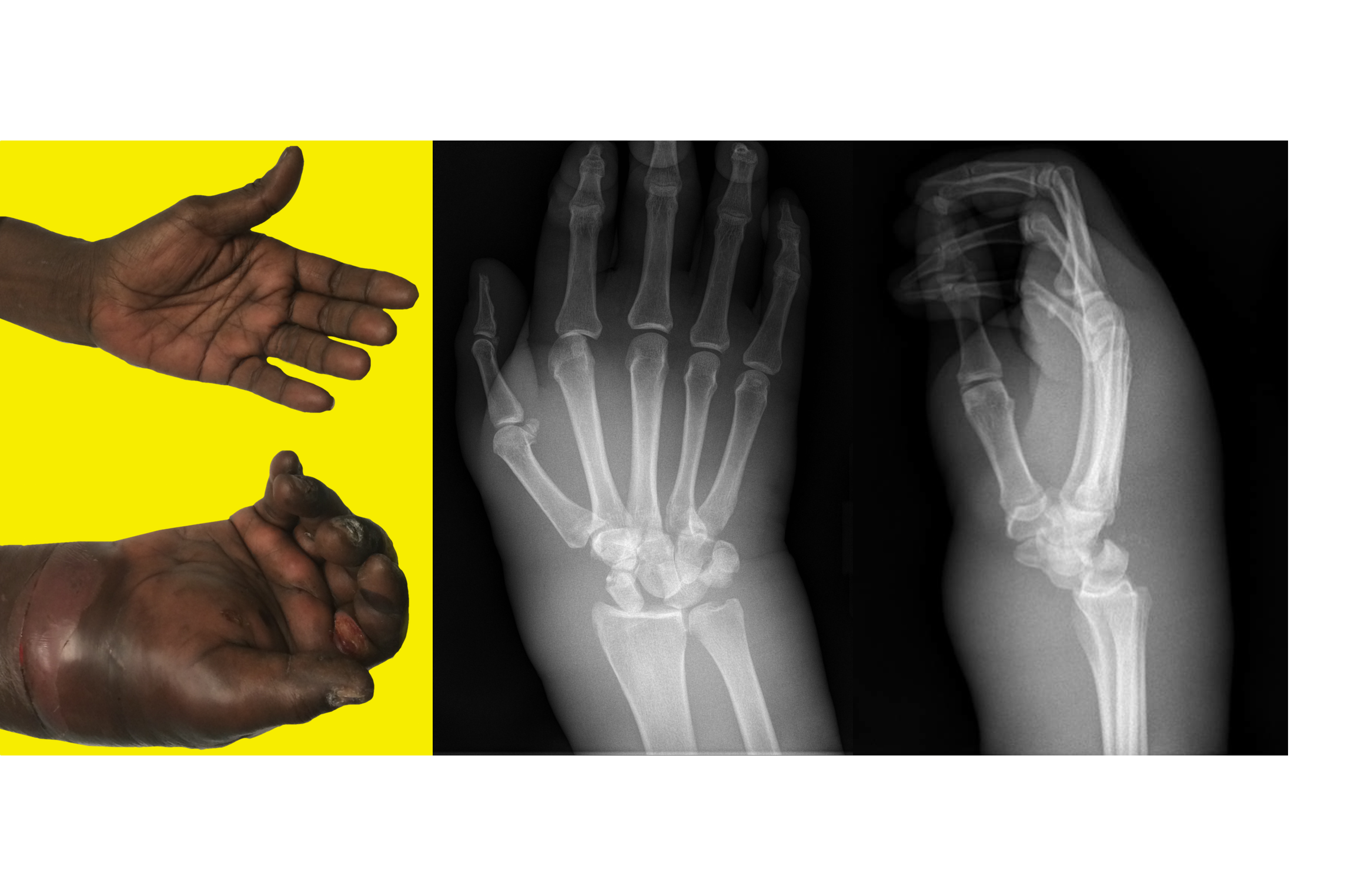
45 year-old right-hand dominant patient presents with right hand pain from a prior injury to hand. Patient has also been injecting subcutaneous heroin into hand for relief. What's the diagnosis?
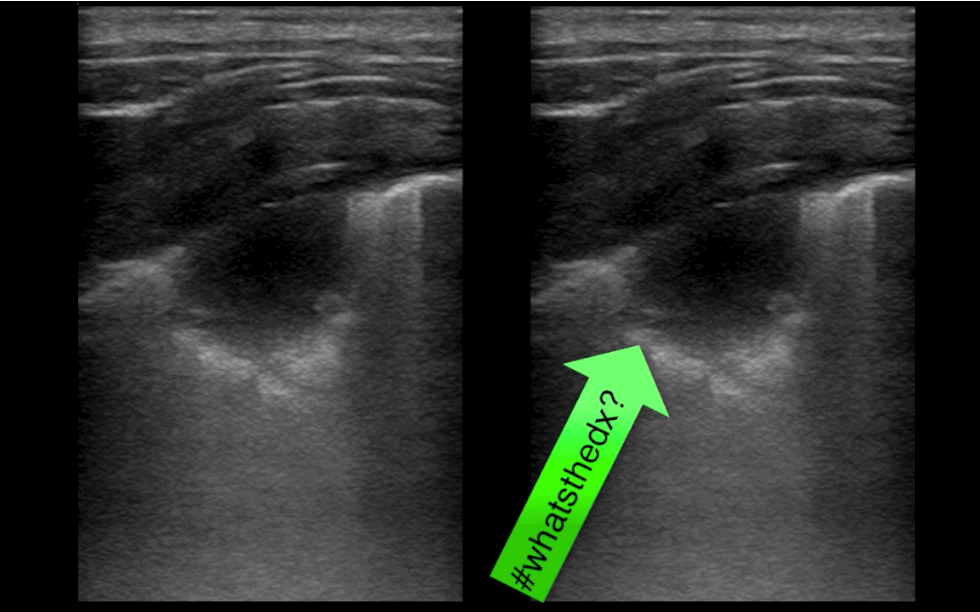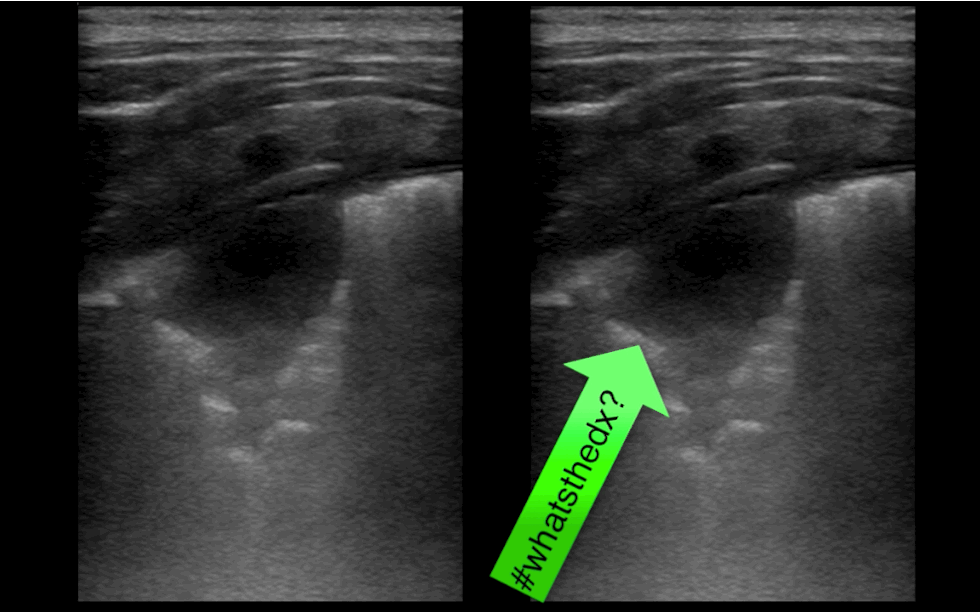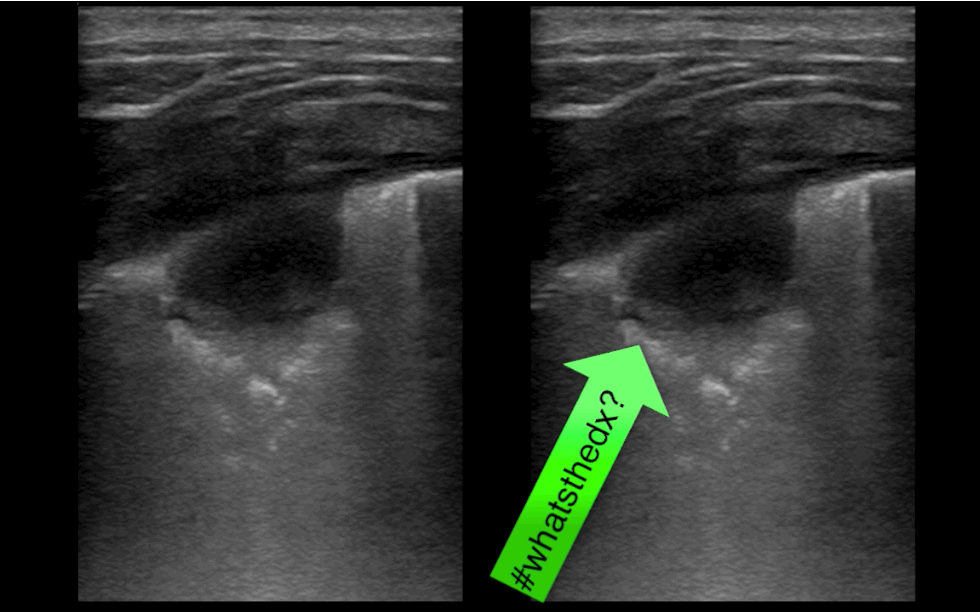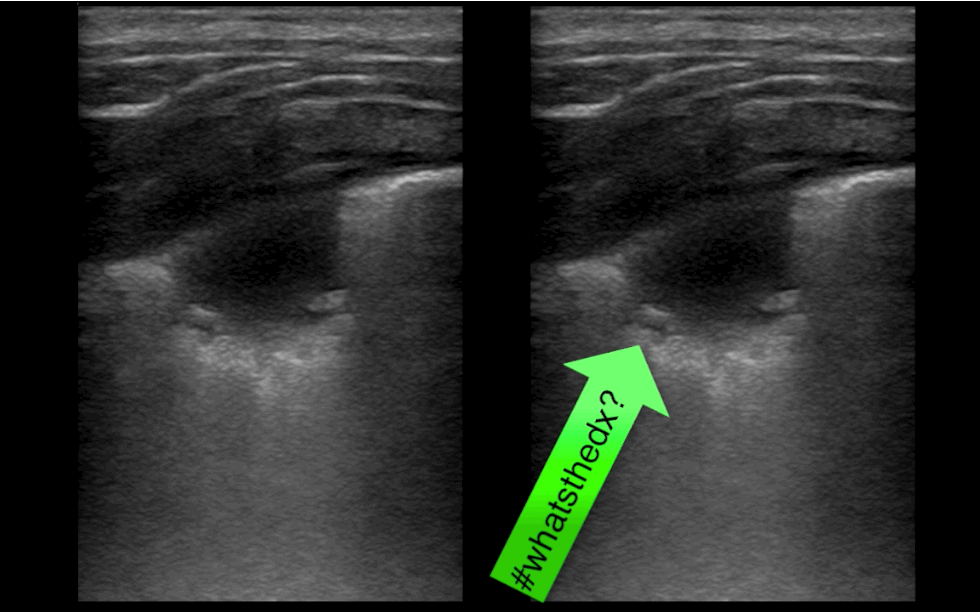
30 year-old presents with cough & fever. CXR shows mild right lower lobe pneumonia. The lung ultrasound of the right lower lobe is shown below. What's the diagnosis?
Editors note: The new Back 2 Basic series will review essential critical care concepts on the first Tuesday of each month. Want a specific topic reviewed? Contact us by email or Twitter.
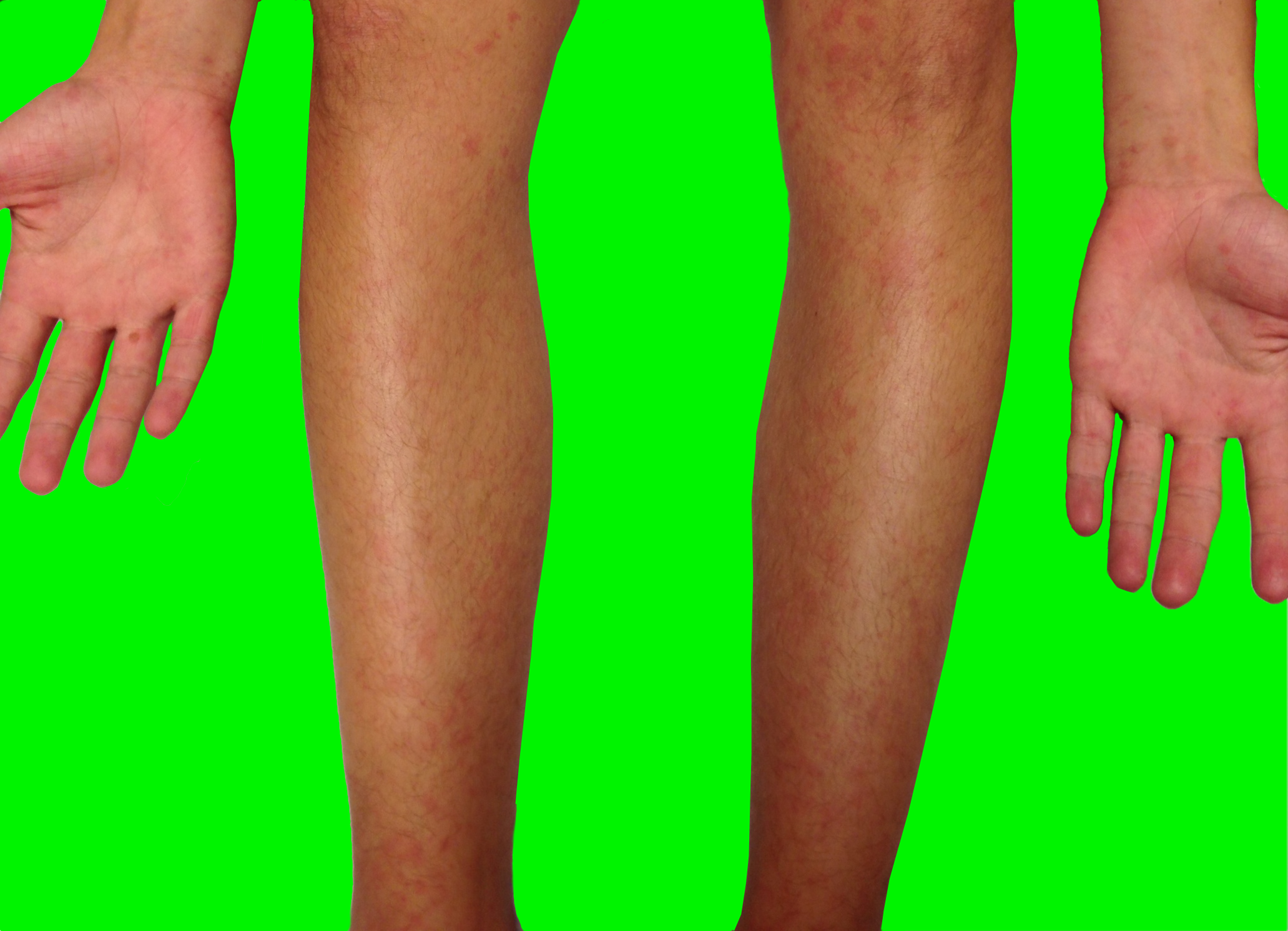
10 year-old male complains of fever and rash (shown below); no other complaints. He went camping 10-days ago. What’s the diagnosis...and what medication(s) should he receive?
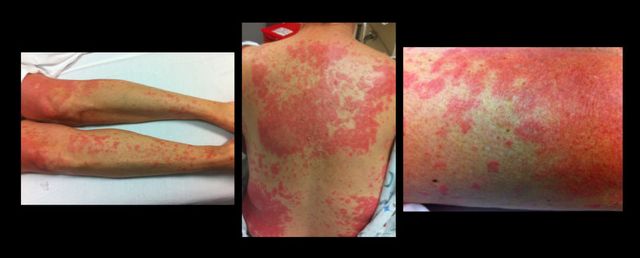
49 year-old female on trimethoprim/sulfamethoxazole presents with a rash & lesions on her oral mucus membranes. What's the diagnosis?
35 year-old female presents with nausea and vomiting 1 week post-op for an abdominal surgery. Abdominal ultrasound is below; what's the diagnosis?
41year-old male without past medical history presents with the image below. What's the diagnosis and what's the most likely causative organism?
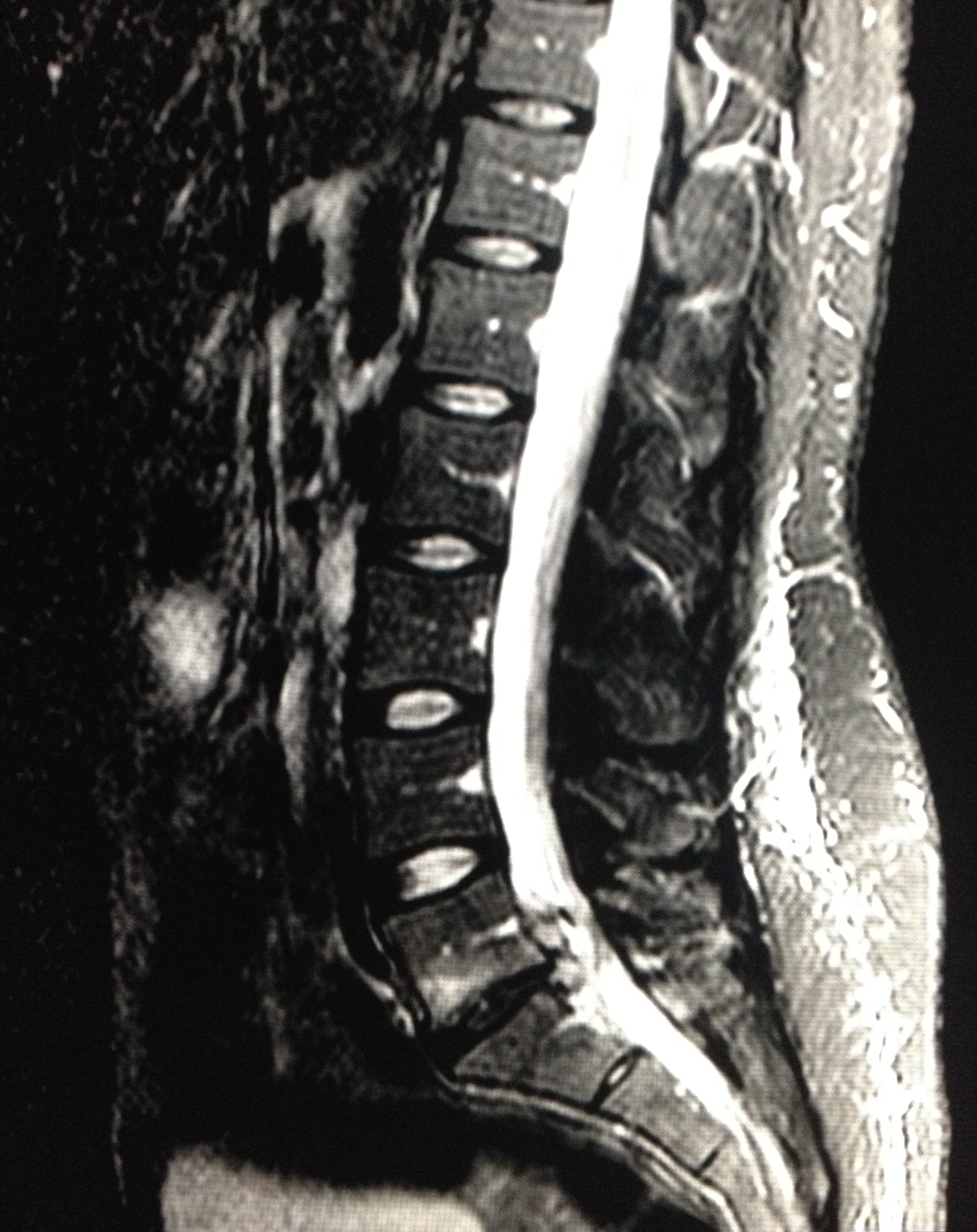
28 year-old female with history of chronic back pain presents with right-foot numbness and inability to move her foot at the ankle joint. What’s the diagnosis and what neurologic finding would you expect to find?
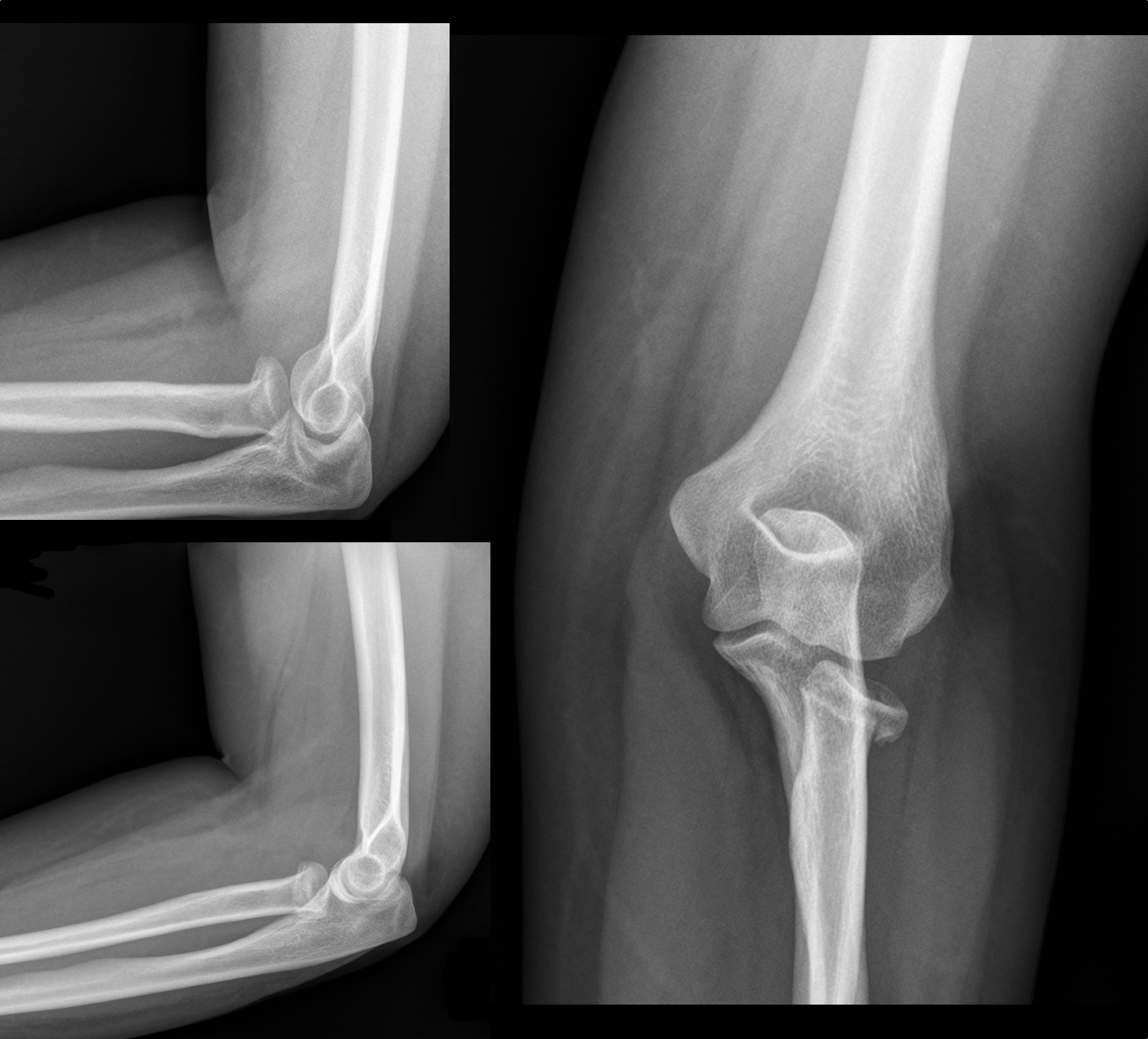
30 year-old female with elbow pain following a fall. What's the diagnosis? (bonus points if you name the fracture with an associated radio-ulnar joint dislocation)
Diabetic patient with active intravenous drug use presents with hypotension, fever, and tenderness of right arm. What's the diagnosis and what antibiotic(s) would you start?